Since the fall and break-up of the Soviet Union, Mongolia’s healthcare has emerged as a free-market healthcare model. It has been struggling to transition from a state-run public healthcare to free market private healthcare enterprise. They have very eager doctors but have been lacking in training & mentorship. The present generation of ophthalmologists are breaking the mould. They have been travelling to other countries to gain expertise and returning to their home country to provide service. They have a genuine thirst for international interaction and collaboration.
Tag Archives: Ophthalmology
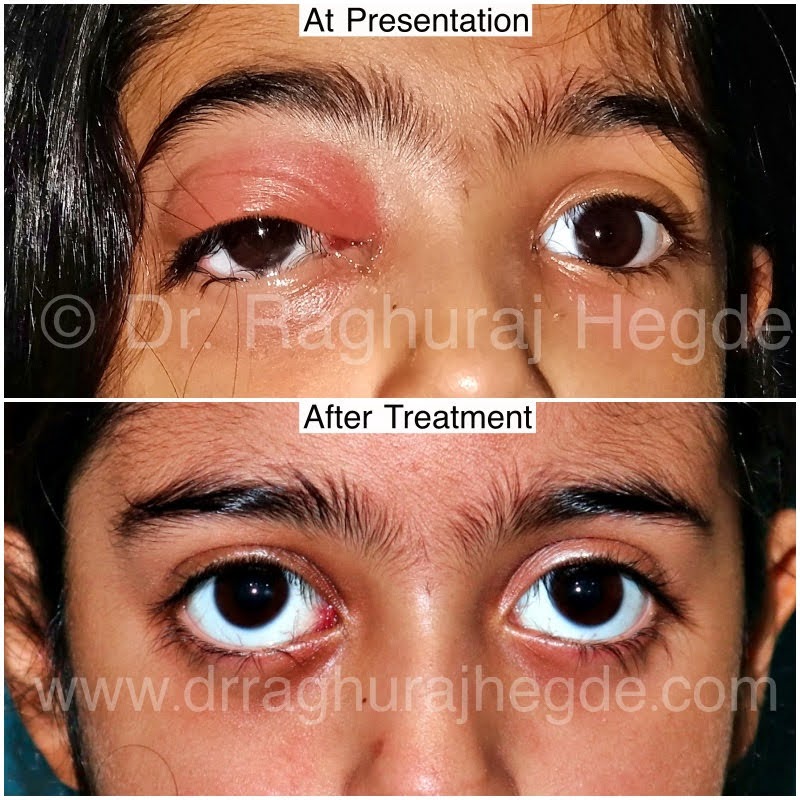
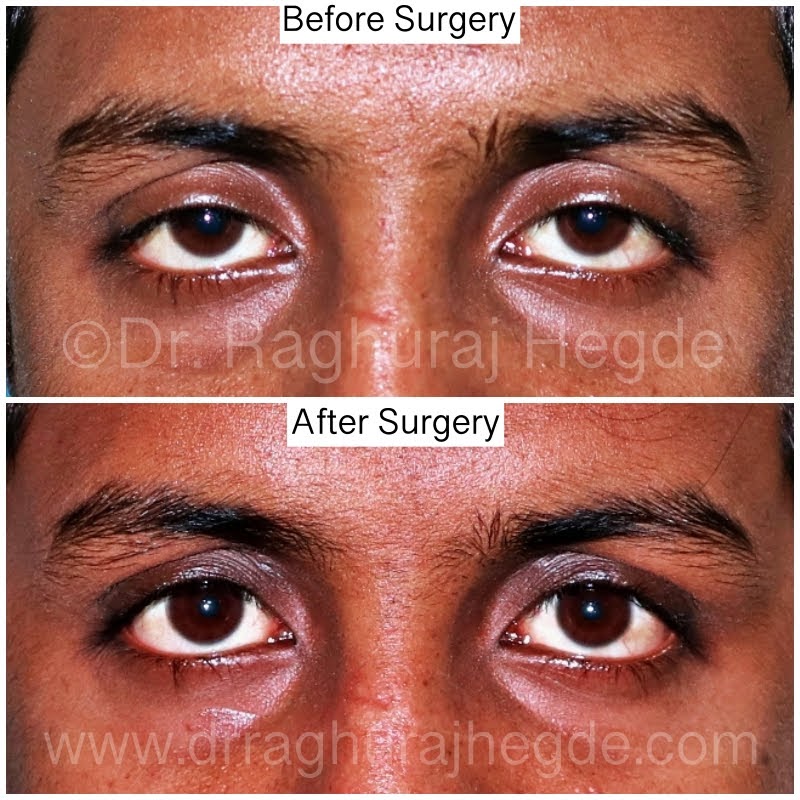
How do you correct hereditary acquired droopy eyelids?
Chronic progressive external ophthalmoplegia (CPEO) describes an spectrum of hereditary myopathies affecting extraocular muscles (EOMs) commonly manifesting as bilateral ptosis and near total external ophthalmoplegia.
As the name suggests, it is a chronic, progressive, bilateral, typically symmetric, and external (i.e., spares the pupil) ophthalmoplegia. CPEO is associated with mitochondrial disease and can occur as isolated oculomotor symptoms (isolated CPEO) or in conjunction with other systemic findings (“CPEO-plus”). Depending on additional clinical features, CPEO can be evaluated as part of a systemic myopathic or neurologic syndrome
It seems like Magic but it’s NOT!
Ocular Surface Squamous Neoplasia (OSSN) is a spectrum of pre-cancerous and cancerous lesions of the conjunctival epithelium (transparent coat covering the surface of the eye).
This condition can be diagnosed clinically and if promptly treated can achieve complete cure.
Happy tears!
A #Customized ocular prosthesis (prosthetic eye) 👁️ surgery is considered when we have to remove an #eye due to one of the following reasons:
1. Eye Cancer (for example Retinoblastoma in children)
2. Irreparable eye injury due to trauma (children & adults)
3. Cosmetically disfigured eyeball with no hope of visual rehabilitation and which may or may not be painful.
Eyes don’t see what the mind doesn’t know!
It is not often that an eye surgeon is able to awe a room full of medical students and residents in a busy Ophthalmology clinic. So I’ll take this opportunity to write the story about this this extra-ordinary accomplishment.
Catching the Moving Lid!
Ocular Myasthenia Gravis (OMG) is one of the conditions that an oculoplastic surgeon can correct without surgery or any invasive intervention. It is a very satisfying to treat a patient of OMG provided the diagnosis is accurate. It has the rare distinction of being both under-diagnosed and over-investigated in different settings. Clinical examination is the cornerstone of a diagnosis of OMG. The various fancy but expensive testing can only corroborate a strong clinical suspicion
Dangers Lurking Around the Eye
Eye is surrounded by the Para-nasal sinuses. In children, the sinuses are small and they increase in size as the child grows. Children are vulnerable to sinus infections as a consequence of upper respiratory tract infections reducing the ciliary clearance from the sinuses and fluid stasis. Sinus infections in turn can be dangerous to the eyes as the distance between sinuses and eye is very small in children especially the medial walls of the orbits which is paper thin aptly named- lamina paprycea.
Where is the scar?
I always remember my mentor’s words while I was closing up during surgery during my fellowship, “You may do the most complicated surgery in the most beautiful way possible but the patient will judge the surgery by the scar you leave behind” This maxim has been drilled into me- so much so that my residents find me being too anal about wound closures. I spend extra time being careful about how I close wounds.
Your eyes reflects your personality
Ptosis can be easily treated with a day care, single sitting surgery and sometimes there need not even be a external skin incision. The surgery is known as conjunctivo-mullerectomy where the ptosis (droopy eyelid) is corrected using an incision on the wet surface of the eyelid.
Riding up the Lower lid!
Entropion is in common language inward turning of the eyelid margin. This causes trichiasis (lash-cornea touch), where the eyelashes are directed inwards toward the globe. This malposition can cause corneal irritation due to constant touch by the lashes.