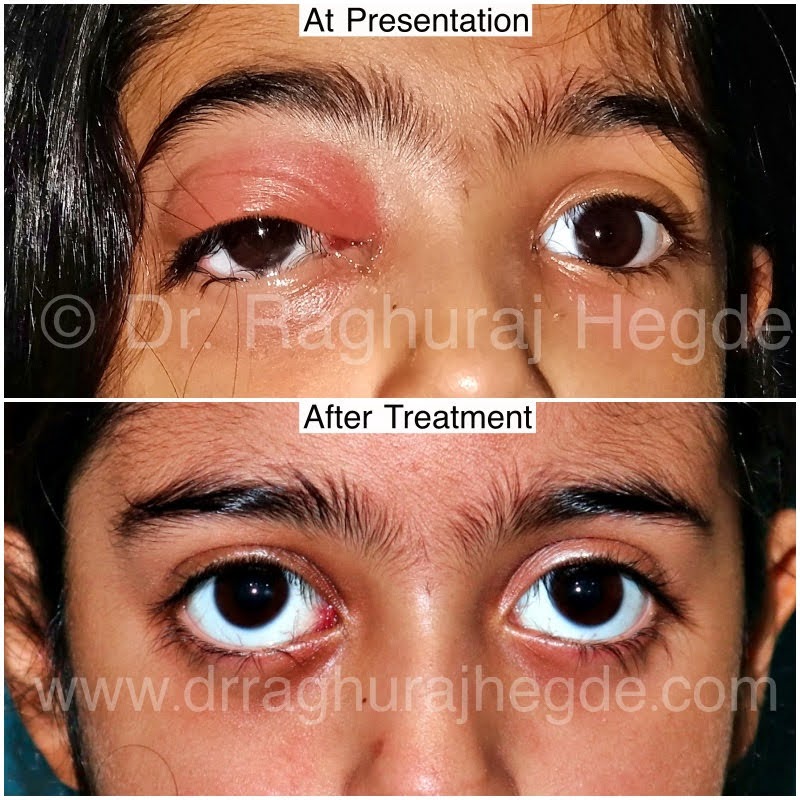
Eye is surrounded by the Para-nasal sinuses. In children, the sinuses are small and they increase in size as the child grows. Children are vulnerable to sinus infections as a consequence of upper respiratory tract infections reducing the ciliary clearance from the sinuses and fluid stasis. Sinus infections in turn can be dangerous to the eyes as the distance between sinuses and eye is very small in children especially the medial walls of the orbits which is paper thin aptly named- lamina paprycea.
Tag Archives: Orbitotomy
A Lot to cry about…… but finally tears of happiness!
Once the incision wound had completely healed, it was like he never had a surgery. Even the patient himself couldn’t locate the scar. The is the benefit of a minimally invasive surgery and aesthetically planned surgery. Even though the entire orbital lobe of the lacrimal gland was excised, there was no dry eye in the patient. This is because most of the regular lacrimation is by minor lacrimal glands spread out throughout the conjunctiva (transparent layer on the eyeball).
Not all masses are tumours!
The histopathology of the mass turned out to be characteristic of tissue infected with Mycobacterium Tuberculosis. In the sub-continent, tuberculosis (TB) is always a differential even when tests for TB turn out to be negative. Histopathology is gold standard for diagnosing TB. Orbital TB though not always a top clinical diagnosis it is not uncommon.
Growing out of a Crack!
Dermoid cyst (also known as choristoma) is a benign tumor growing out of a embryonic suture line. The tumour consists of normal cells occurring in an abnormal location. It is usually diagnosed in children when it is first visible but it is not uncommon to have adults coming to the clinic to know if it can be removed.
Hugging the Optic Nerve!
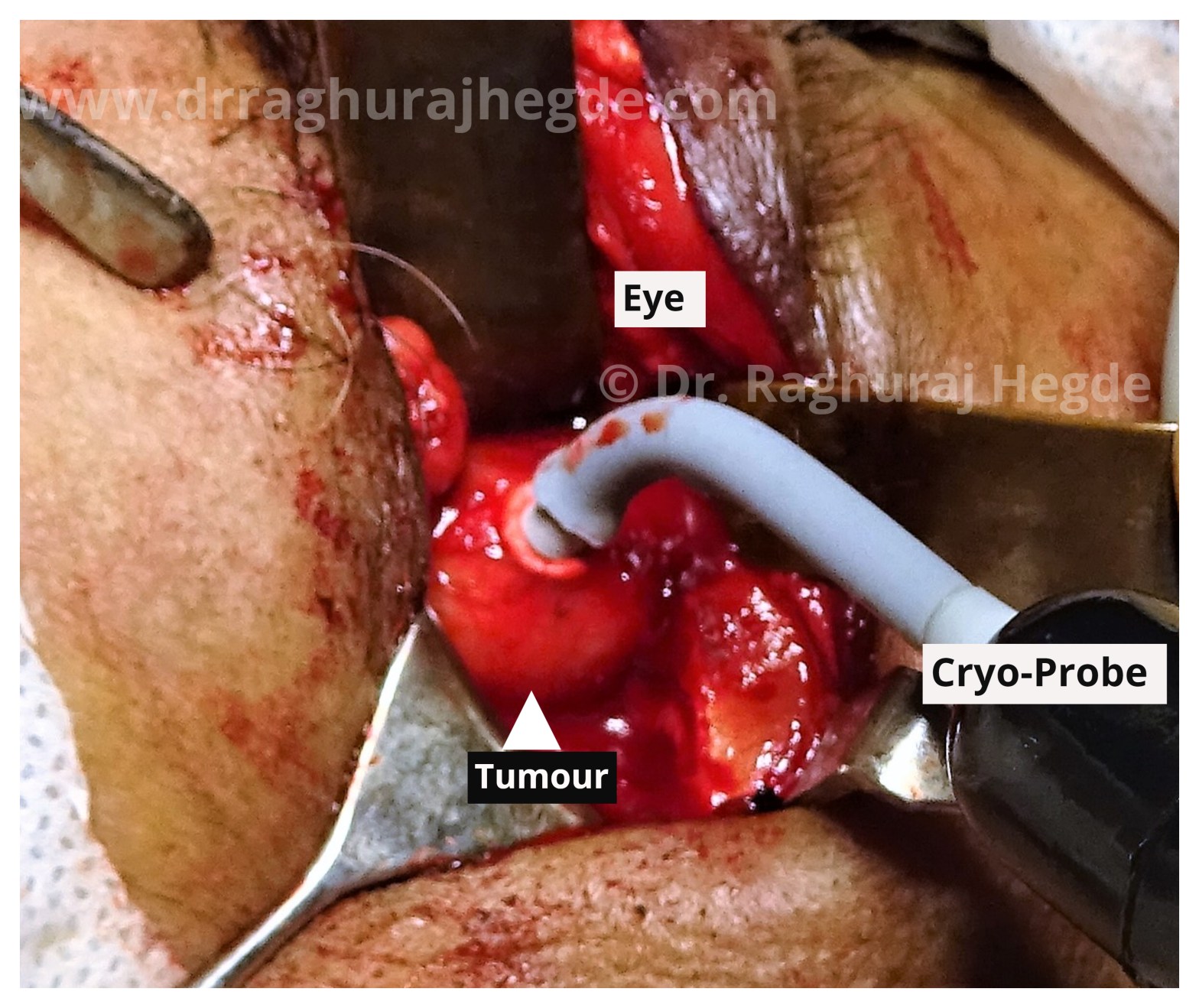
The MRI scan showed a large intraconal well defined mass sitting right next to the optic nerve causing mass effect which in turn was causing diminution of vision. My working differentials going into surgery- based on location and imaging was Cavernous Hemangioma, Fibrous Histiocytoma, Dermoid cyst, Schwannoma among others.
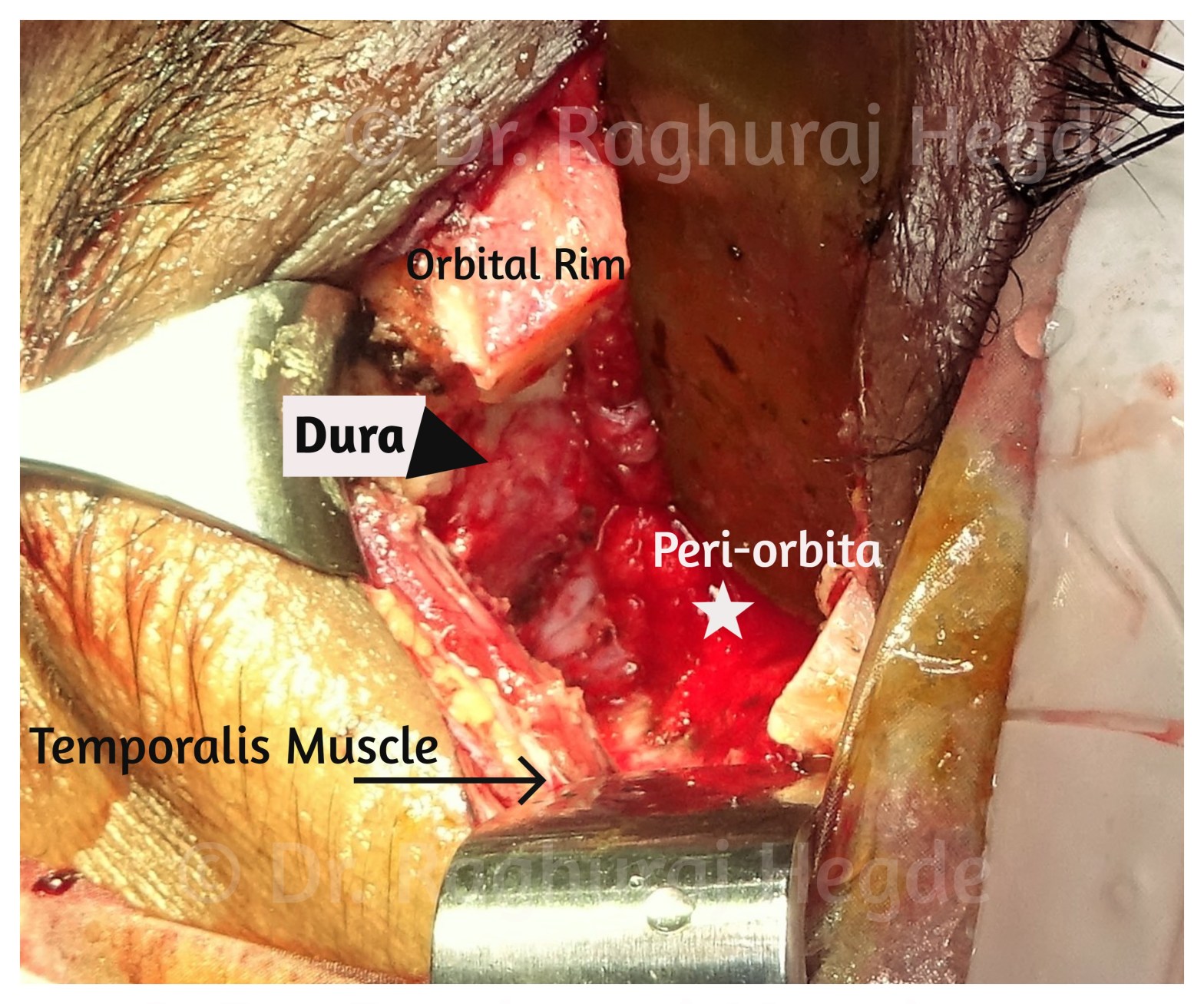
A Bridge between Eye & Brain
Nothing beats the feeling of being able to remove a skull base tumour through a small incision in the upper eyelid crease. This here is after the tumour has been completely excised. This picture shows the amount of exposure we can achieve by just the orbital route and also that’s me admiring the orbital anatomy for a few seconds before closing up.
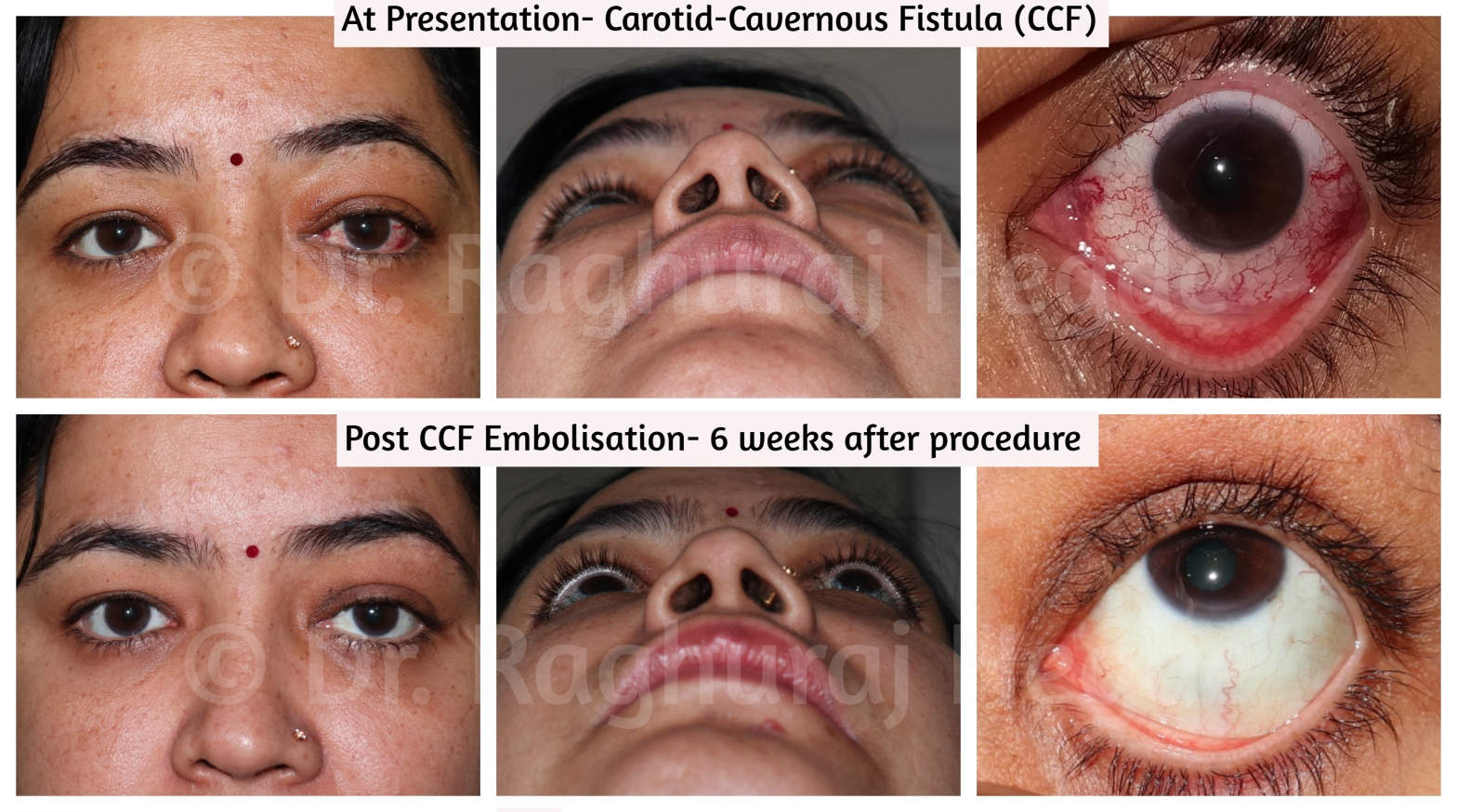
Finding a road to the fistula
It is very rare that oculoplastic surgeons are asked to provide access to interventional neuro-radiologists. This is one such case. We have performed such interventions in 3 cases till date at our hospital with similarly successful outcomes. The important thing to remember as a surgeon while accessing the SOV is that the vein is arterialised due to the CCF and bleeding can be very severe is the vessel wall is damaged.
Tumour Behind the eye! Intra-conal Orbital Cavernous Hemangioma
In an earlier era, these tumours would be removed via a craniotomy (brain surgery) by neurosurgeons or a disfiguring open surgery sometimes causing the loss of vision in the involved eye by other surgeons- that’s way too much morbidity for a benign tumour. But with the advent of modern day techniques and skilled oculoplastic surgeons performing orbitotomy today to remove such tumours, this surgery’s risks and complications is very low with the added advantage of a scarless as well as without even having to remove bone. This surgery is followed by a mostly uneventful recovery period.