Dermoid cyst (also known as choristoma) is a benign tumor growing out of a embryonic suture line. The tumour consists of normal cells occurring in an abnormal location. It is usually diagnosed in children when it is first visible but it is not uncommon to have adults coming to the clinic to know if it can be removed.
Tag Archives: Oncology
Hugging the Optic Nerve!
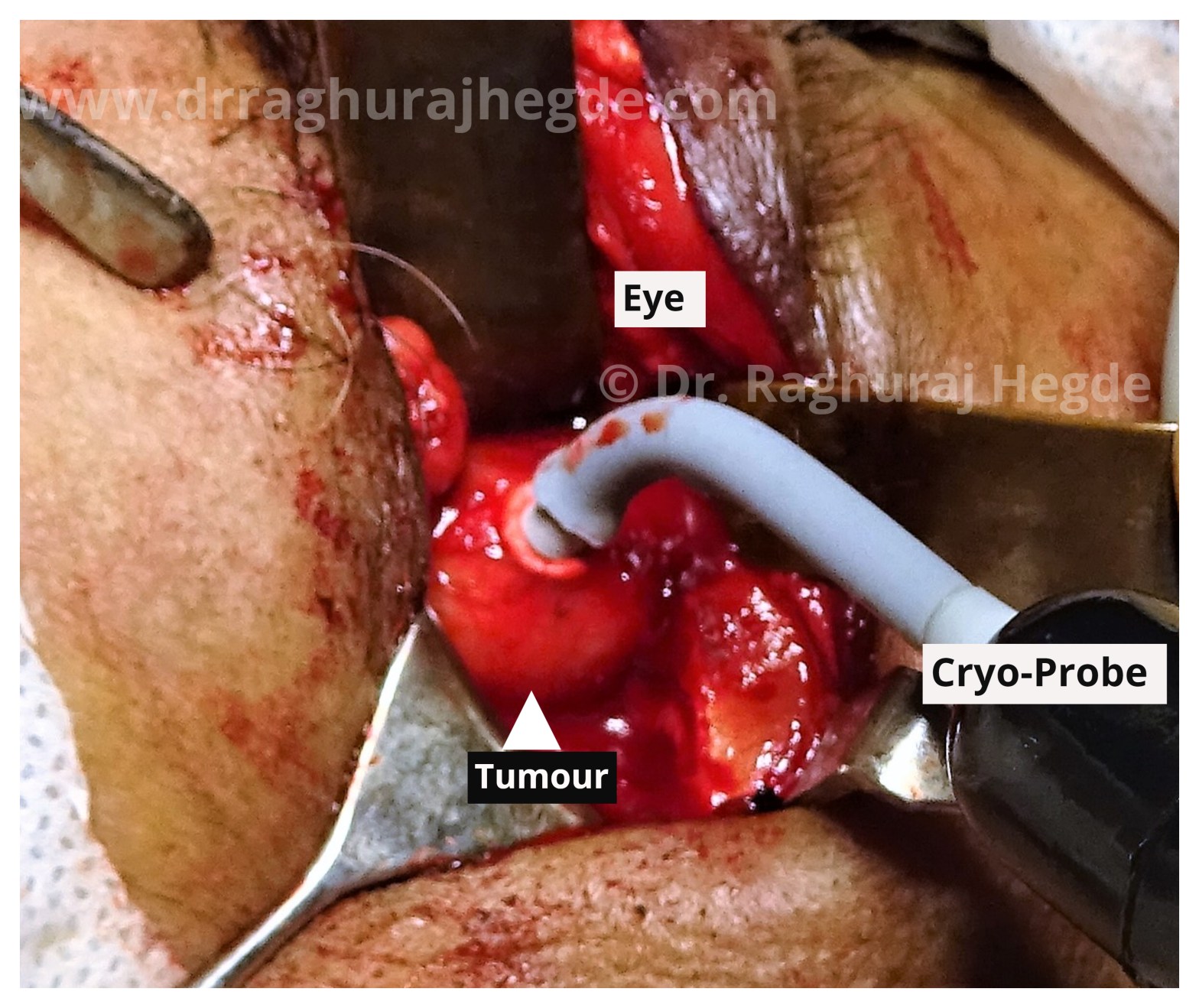
The MRI scan showed a large intraconal well defined mass sitting right next to the optic nerve causing mass effect which in turn was causing diminution of vision. My working differentials going into surgery- based on location and imaging was Cavernous Hemangioma, Fibrous Histiocytoma, Dermoid cyst, Schwannoma among others.
Guidelines for the Oculoplastic and Ophthalmic Trauma Surgeon during the COVID-19 era – An APOTS & APSOPRS Document
The outbreak of COVID-19 pandemic is changing the infection, transmission and safety practices of medical establishments globally. From evidence that is available presently, the risk of transmission of this virus is high amongst medical personnel involved in procedures and surgeries around the head and neck region- Ophthalmology, Otorhinolaryngology, Craniomaxillofacial surgery, Head and Neck Oncology, Neurosurgery including Anesthesiology. The field of Oculoplastic Surgery has risk factors common to both ophthalmology and all of the above craniofacial subspecialties. While clear directives and strategies to handle elective, urgent and emergency surgeries in SARS-Cov2 positive patients is constantly evolving, we herewith attempt to consolidate various guidelines from various relevant professional global medical societies which will be beneficial to the orbit, oculoplastic and ophthalmic trauma surgeon and also their hospital administrators.